Among all the pathological processes affecting the spine in its different parts, cervical osteochondrosis is considered one of the most common. This disease leads to a lot of complications, mainly because it affects the spinal cord and also negatively affects the functioning of the brain.
According to statistics for 2017, the disease has become significantly younger. If previously osteochondrosis mainly affected people after 40 years of age, today various stages of cervical osteochondrosis are diagnosed in 90% of people over 25 years of age. For this reason, it is important to know as much as possible about the pathology, from what it is to treatment methods.
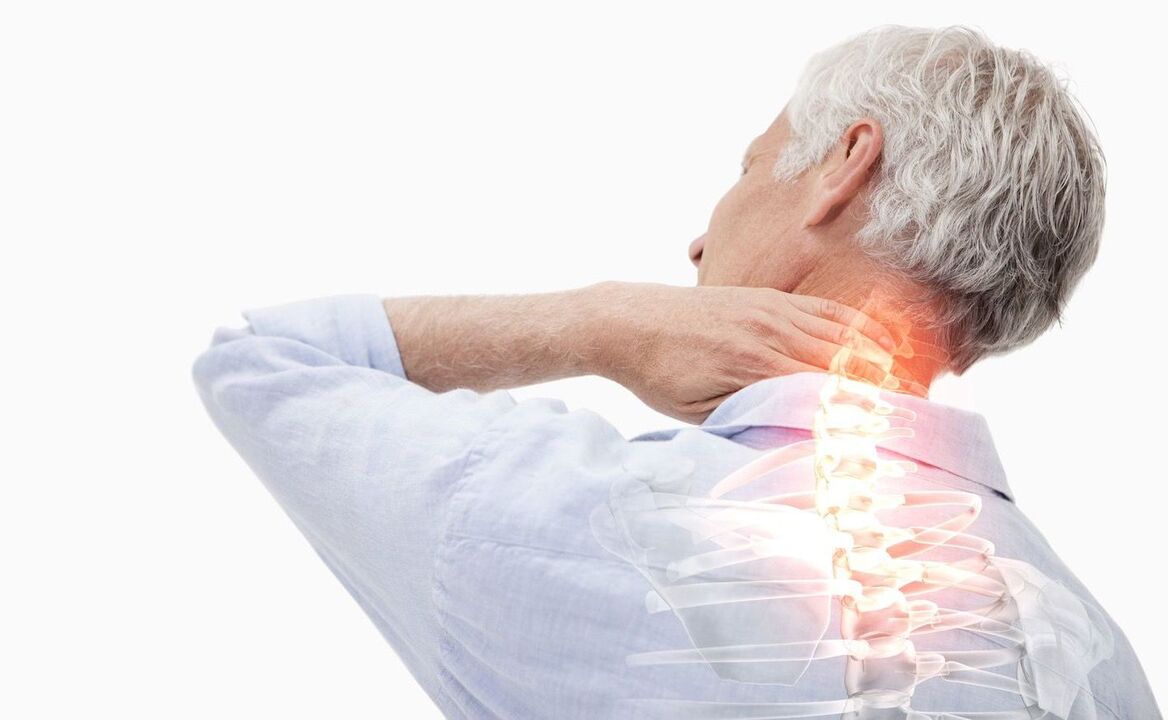
What is cervical osteochondrosis?
In medical practice, the words cervical osteochondrosis mean an acquired progressive disease that affects a specific part of the spine. This pathological process is characterized by degenerative-dystrophic processes in the tissues of the intervertebral discs, which are shock absorbers for the cervical vertebrae.
Degenerative-dystrophic changes in the intervertebral discs are caused by the fact that they are worn out and deformed. As a result, the distance between the vertebrae is reduced and as a result the following consequences occur:

- Narrowing of the spinal canal in certain areas of the spine.
- Compression of the vertebral arteries - large blood vessels that provide blood supply to the brain. Because of this, the supply to the brain deteriorates and blood circulation in the cervical spinal cord is disrupted.
- Intervertebral discs can become deformed and flattened. This leads to compression of certain areas of the spinal cord and nerves, most often compression of the nerve roots occurs.
All of these problems threaten not only impaired blood circulation in the brain, pain in the neck, headaches, etc. The development of osteochondrosis of the cervical spine is dangerous with neurological problems, deterioration of the central nervous system, and damage to brain tissue.
According to the international classification of diseases, osteochondrosis of the cervical spine is assigned several separate codes. The disease code according to ICD 10 depends on the age at which the disease was diagnosed:
- M02 – dystrophy of intervertebral discs in adolescence.
- M42. 12 – degenerative process in the neck area in adults.
A lot of factors depend on the age of the patient and the degree of development of the pathological process, for example, consequences, complications, symptoms and, of course, principles of treatment.
Causes
Knowledge of the causes of the development of cervical osteochondrosis can play a decisive role in the diagnostic process, as well as in determining the principles of combating the disease.
However, before listing the reasons, it is worth saying that doctors identify two factors that lead to the development of this pathological process:
- Pathological - destruction of intervertebral discs and other vertebral structures with the involvement of nearby tissues, vessels and nerve bundles in the pathological process occurs under the influence of unfavorable external factors. The more severe these factors and other pathologies are, the faster the disease develops.
- Physiological – the development of pathology is based primarily on age-related changes. We are talking about the natural aging of cartilage tissue in the spinal column, salt deposits, etc.
If we list more specific causes of cervical osteochondrosis, they are as follows:
- Disorders of metabolic processes in the body, as well as certain stages of obesity.
- Physical inactivity is a phenomenon characterized by limited mobility. We are not just talking about injuries or illnesses, this also includes a sedentary lifestyle and sedentary work.
- Pathologies of the cardiovascular system that contribute to impaired blood circulation in the brain, pressure changes, etc.
- Incorrect posture includes various forms of scoliosis, rheumatism and even flat feet.
- Injury to the cervical spine. In this case we are talking about sprains, blows, bruises. Injuries to other parts of the spine can affect the development of cervical osteochondrosis.
- Excessive physical stress on the cervical spine, caused by intense sports or severe physical difficulty, depending on the type of person’s activity.
- A sedentary lifestyle is also dangerous due to constant tension in the cervical spine and the entire spine if you sit incorrectly or on uncomfortable furniture.
- Hernia of the cervical spine, as well as various concomitant diseases.
- Forced holding of the head for a long time in an uncomfortable or unnatural position. In this case, not only muscle strain occurs, but also the spine in the cervical region is bent.
- Doctors consider constant stress and nervous tension to be a very common cause.
- One of the reasons is also considered to be congenital anomalies in the structure of the spine.

What health hazards does it pose?
As mentioned earlier, the cervical spine region contains not only the spinal cord and various nerve branches, but also the vertebral arteries that supply blood to the occipital part of the brain, the cerebellum and the medulla oblongata.
With the development of cervical osteochondrosis, nearby tissues become inflamed. In addition, the development of pathology threatens to compress nerve roots and squeeze blood vessels, the consequences of which are as follows:
- Osteochondrosis is accompanied by spinal deformities, resulting in narrowing of the spinal canal in certain areas. This can lead to compression of the spinal cord and nerve branches, which promises severe neurological problems. In severe cases, a person feels pain, and there is even a possibility of loss of control over certain parts of the body (mainly in the arms or face).
- Compression of the vessels of the neck, as already mentioned, is accompanied by impaired circulation in the occipital region of the brain. In this case, the brain stops receiving oxygen and nutrients in the required quantities, and oxygen starvation begins. If blood circulation is impaired, there is a real risk of ischemic stroke and various neurological pathologies.
Syndromes
Speaking about the danger that cervical osteochondrosis poses as it progresses and lacks proper treatment, the disease can lead to a number of complications and syndromes.
The main syndromes are:
- Vertebral.
- Vertebral artery.
- Koreshkovy.
- Cardiac.
It is important to know that each of these symptoms is accompanied by painful sensations of a different nature, as well as a host of unfavorable clinical signs. A person may feel dizzy, have tinnitus, and much more.
Vertebral syndrome
Speaks of a direct connection between cervical osteochondrosis and bone and cartilage tissues. Symptoms of this type of pathology are also associated with damage to the mentioned tissues:
- Neck movements are partially or completely limited.
- Head movements are accompanied by painful sensations in the neck area.
- X-ray shows morphological changes in tissues (intervertebral and vertebral bodies).
It is worth noting that vertebral syndrome is always accompanied by these three clinical signs. If at least 1 of them is missing, the diagnosis will be completely different.
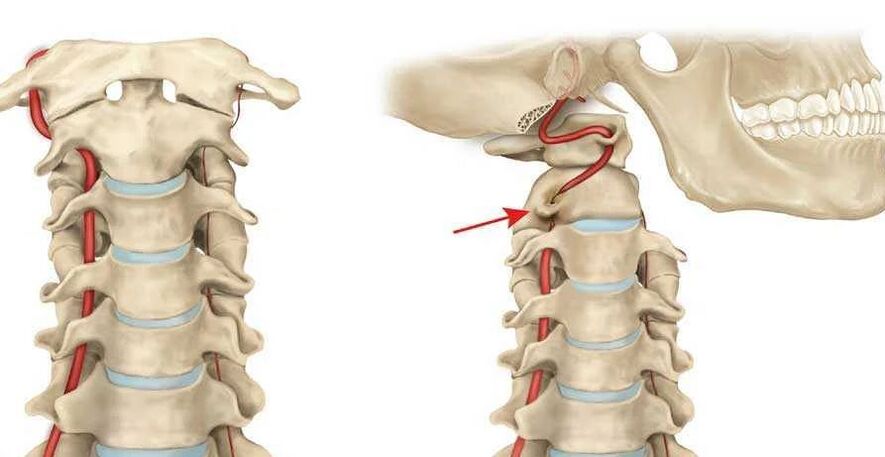
Vertebral artery syndrome
This syndrome is caused by a narrowing of the vertebral artery, which leads to vestibular, vascular and autonomic problems. In this case, the main symptoms are extensive:
- Headaches and migraines.
- Visual impairment.
- Noises in the ears.
- Frequent dizziness and much more.
The most dangerous symptom is fainting, which indicates severe oxygen deprivation.
Radicular syndrome
Occurs when the roots of the spinal cord are damaged. In this case, nerve conduction is disrupted, a person may feel pain or lose sensitivity in certain parts of the body, or even suffer from paralysis.
Depending on which of the 8 radicular pairs the conduction disturbance occurs, the following symptoms are identified:
- 1 pair – numbness or pain in the back of the head;
- 3rd pair – impaired chewing reflex, numbness of the tongue and unpleasant sensations behind the ears;
- 4 pairs – pain in the collarbone area, impaired swallowing reflex;
- 5 pair – disorders of the shoulder girdle, accompanied by problems with arm movement;
- 6th pair - the patient begins to feel pain and numbness in the forearm and shoulder blades;
- 7th pair – hands and fingers (usually index and middle) go numb;
- 8th pair – problems similar to the previous point, but numbness is felt in the ring finger and little finger.
Based on the described features, it is sometimes possible to determine which pair of roots is affected by radicular syndrome.
Cardiac syndrome
Despite the fact that the pathological process is still localized in the cervical spine, the syndrome has all the signs of cardiac pathologies. The clinical picture is as follows:
- Rapid pulse.
- Pain in the sternum.
- Shortness of breath, weakness, lethargy, decreased performance.
Degree of disease development
When talking about the degree of osteochondrosis of the cervical spine, we mean the stages of progression of the pathological process, which differ in clinical signs. In total, there are four degrees of development of the disease:
- The first stage is characterized by vague symptoms. Patients complain of minor headaches; during the initial examination, the doctor notes a slight degree of muscle stiffness.
- Pain in the cervical spine and head is more common, more intense, and radiates to the shoulder and arms. The pathology is caused by damage to the intervertebral discs and pinched nerve roots. The pain intensifies when turning the head, throwing it back and bending forward.
- At the third stage, the pain is constant, muscle weakness in the arms is noted, and hernias form in the intervertebral discs. Movements in the neck area are constrained, and frequent dizziness is present.
- The fourth stage is accompanied by complete destruction of the intervertebral disc, cartilage tissue is replaced by connective tissue. In addition to pain and dizziness, coordination problems are observed, and the vertebral arteries are often pinched.
Signs and symptoms of cervical osteochondrosis
To consult a doctor in a timely manner, it is necessary to clearly understand the signs of cervical osteochondrosis. In some cases, such knowledge allows you to seek help in the initial stages of the disease, when it is easier to treat.
In general, the symptoms of osteochondrosis of the cervical spine are as follows:
- Pain in osteochondrosis is always present, only the intensity and frequency differ. Pain is the first clinical sign. Their intensity depends on the stage of progression of the disease; they are dull or compressive in nature. Painful sensations are present mainly in the neck and occipital region, but can also radiate to the temporal region, shoulder girdle and arms.
- In most cases, there are manifestations of damage to the vestibular apparatus. We are talking about frequent causeless dizziness, nausea, poor coordination of movements, uneven gait, loss of space.
- One of the most common clinical signs is stiffness of the neck muscles and stiffness of movement. It is difficult for a person to turn, lower and throw back his head, movements are accompanied by attacks of pain.
- Many patients report a feeling of "goosebumps" running across the scalp or a characteristic tingling sensation.
- Muscle weakness and numbness occur in the arm area.
- Often there are psychological manifestations, expressed in depression, drowsiness, sudden changes in mood, short temper or irritability.
- Due to poor circulation and damage to brain tissue, dizziness intensifies and noise in the ears appears, similar to rustling, pulsation, and ringing.
- Most patients note deterioration in vision, as well as pain in the eyeballs, especially when trying to squint their eyes too much to the left, right, up or down.
It is sometimes possible to determine the degree of development of the pathological process by symptoms. However, for a full diagnosis this is still not enough and a number of diagnostic measures are required.
Diagnostic methods
Diagnosis of cervical osteochondrosis is necessary to determine the location and stage of progression of the disease. For a complete diagnosis, the following diagnostic methods are needed:
- Radiography is the primary method for determining the degree and location of spinal column deformity.
- Computed tomography can be used to more accurately diagnose pathological changes in the vertebrae and intervertebral discs.
- MRI (magnetic resonance imaging) - makes it possible to examine discs and vertebrae in detail, determine the presence of hernias, protrusions, the extent of lesions, etc.
- Dopplerography - with this examination it becomes possible to find the place of compression of the artery and assess the degree of circulatory disorders.
Treatment methods
Treatment of neck osteochondrosis always involves an integrated approach. The principles of treatment depend on a host of factors, such as the patient’s age, the stage of development of the disease, the severity of the clinical picture, etc.
Nevertheless, you cannot do without a doctor in this situation and first of all you can contact a general practitioner, who will then refer you to a vertebrologist.
As for the integrated approach: osteochondrosis of the cervical spine is treated with the help of drug therapy, physiotherapy, massages, exercise therapy and other methods, which are worth talking about in more detail.
Drug treatment
The basis for the treatment of cervical osteochondrosis is drug therapy, which involves the use of tablets, drugs and medications of the following groups:

- Painkillers - analgesics and antispasmodics. The first ones directly dull the nerve centers, thereby relieving painful sensations. The latter allow you to relieve spasm of the neck muscles, improving blood flow and suppressing pain.
- NSAIDs - non-steroidal anti-inflammatory drugs are necessary to reduce inflammation, most of them also eliminate pain. Often these medications are used in the form of gels or ointments that are rubbed into the affected area.
- Muscle relaxants are another way to relieve muscle spasms in the cervical region.
- Chondroprotectors are mandatory at certain stages of osteochondrosis of the spine, because they contribute to the restoration of bone tissue.
- B vitamins - normalize the metabolic processes of nerve tissue, improving the conductivity of nerve impulses and promoting the functioning of the central nervous system.
Remember, treatment should only be carried out under the supervision of a doctor, who is responsible for prescribing each medication, as well as determining the duration of its use and dosage.
Physiotherapy
Treatment of neck osteochondrosis will be many times more effective using certain physiotherapy techniques:
- Electrophoresis.
- Laser therapy.
- Ultrasound.
- Massage.
Massage therapy must be carried out by an experienced medical professional, treatment is carried out in a course of at least 10 sessions. Cervical massages help normalize blood circulation, restore elasticity, muscle tone, relieve pain, etc.
Physiotherapy
Therapeutic exercises also help speed up recovery, but are carried out only during the recovery stages. It is important that the exercises do not bring discomfort or pain to the patient. Exercise therapy is aimed at strengthening muscles and relieving discomfort during movements by increasing the elasticity of muscle fibers.
The exercise technique is initially developed by a physiotherapist, then the patient can independently perform gymnastics at home.
Manual therapy
Manual therapy is based on the principle of restoring motor functions and mobility between the vertebrae. Initially, the manipulations consist of a light relaxing massage, then the doctor applies more and more force, applying pressure and turning the neck to the vertebrae.
Kuznetsov applicator
The use of Kuznetsov applicators is one of the methods of treating spinal diseases, including osteochondrosis. The effect of the device on the cervical spine normalizes metabolic processes, relieves pain, increases muscle tone, improves blood circulation, increases the conductivity of nervous tissue, etc.
Treatment at home
The entire range of therapeutic measures is carried out at home, with the exception of physiotherapy, massages (in some cases) and the first stages of exercise therapy. However, now we are talking about traditional medicine, and we will consider several of the most effective recipes:
- To use horseradish - take a leaf of this plant, pour boiling water over it and apply the inside to your neck, securing it with a bandage. Can be left on while you sleep to enhance the effect.
- If there are no contraindications from a doctor, warming up the cervical spine would be a good remedy. The simplest method is to use a pepper plaster, but you can heat the wax cake, applying it 1-2 times until it cools completely.
Disease prevention
To prevent the development of the disease or its return after treatment, it is necessary to prevent osteochondrosis of the cervical spine. It consists of following simple recommendations:
- Sleep on a flat, hard surface; it is better to purchase a special orthopedic mattress and a pillow that takes the shape of your head.
- To prevent the disease, monitor your physical activity and do not overstrain your spine. If you have to lift weights, do it smoothly and keep your back straight.
- If your job requires you to sit for a long time, take breaks. Every hour you need to walk or stretch your stiff muscles with simple gymnastic movements.
To prevent osteochondrosis, it is useful to go swimming and hang on the horizontal bar for 2-3 minutes every day.
























